Provider & Staff Education: Level 3
Expand organization’s vaccination expertise
Equip more people with advanced knowledge and skills by scaling up existing educational opportunities for providers and staff across the organization. Consider who can help advance your immunization goals at the clinic and organizational level—including new roles and specialties as appropriate—and explore opportunities to provide these professionals with specialized education and training.
Once staff and provider education around adult immunizations is well established at your organization, look for the following opportunities to expand your immunization expertise.
Expand expertise across roles, specialties, and locations
First, look for opportunities to expand vaccination expertise at the clinic level. Start with any recommended roles in the Getting Started Checklist, such as a pharmacists and pulmonologists, who are not already on your vaccination team. Some groups have found success by hiring vaccine-specific roles, such as a vaccine specialist with in-depth knowledge of immunizations to lead the organization’s immunization program or a vaccine coordinator who is responsible for vaccine management (e.g., ordering, receiving, storing, monitoring temperatures, etc.).
Next, expand your multidisciplinary vaccination team to include roles that can impact care at the system level. Consider adding roles included in the Getting Starting Checklist that were outside of your initial core team or expand to new areas entirely:
- Leadership roles such as the Chief Medical Officer, Chief Quality Officer, and/or Chief Nursing Officer can prioritize immunizations in strategic planning.
- Staff involved in quality metrics and data collection/management (e.g., IT support, quality managers, etc.) can understand how to leverage data to improve vaccination rates throughout the organization.
- Staff involved in procurement, coding, reimbursement, and other areas of business and clinical support can streamline operations across clinics.
Additionally, look for opportunities to engage specialties—like oncology, hematology, and immunology—to close gaps in care. For example, if vaccination rates are lagging in older patients, consider expanding vaccine education to geriatrics and rheumatology departments. Alternatively, if patients with diabetes are a special focus, consider adding endocrinology and preventive medicine to staff and provider training efforts.
With these additional team members engaged, explore tactics for creating an infrastructure and culture to support immunizations at the system level:
- Establish a committee(s) to spearhead immunization activities across locations. These entities can inform staff education, roles and responsibilities, training opportunities, and other areas for growth.
- Foster an organizational culture that prioritizes routine adult immunizations and encourages “no missed opportunities” to vaccinate.
- If applicable, expand programming geographically to gradually increase the number and type (e.g., outpatient clinic, hospital, skilled nursing facility) of sites engaged in your immunization activities.
Leverage new learning opportunities
Once you have appropriate stakeholders engaged and infrastructure in place, look to tools and resources, such as those listed below, to maintain and further develop your teams’ knowledge and skills.
Explore relevant trainings and programs. Consider “train the trainer” programs that provide in-depth education on all aspects of vaccinating a patient, from contraindications to storage and handling. Trained individuals then serve as organization-wide resources for patients and staff with questions. (See below for related tools such as the Immunizations Champions, Advocates, and Mentors Program (ICAMP).)
Participate in conferences. Examples include the National Adult and Influenza Immunization Summit and the National Immunization Conference as well as community collaboratives and forums.
Leverage offerings like webinars for education on complex subjects. Examples of complicated topics include protocols for pregnant patients, guidance for immunocompromised (high risk) and immunocompetent (at risk) patients, protocols for patients with contraindications, and recommendations for unique patient scenarios (e.g., when to give FluMist to adults, whether to immunize a patient when they are sick).
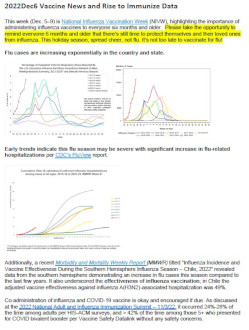
Vaccine Newsletter
Lehigh Valley Physician Group
Showcases an example of an internal weekly vaccine newsletter sent within a medical group to keep providers and staff informed of national vaccine activities.
View Tool
Immunization Champions, Advocates, and Mentors Program (ICAMP) Factsheet
The Gerontological Society of America (GSA)
Provides an overview of Immunization Champions, Advocates, and Mentors Program (ICAMP), a multidisciplinary training program designed to equip healthcare professionals to champion adult immunization practices that improve public health and the quality of care for the people they serve.
View Tool-Summary.PNG?ext=.png)
National Adult and Influenza Immunization Summit (NAIIS) Summary
National Adult and Influenza Immunization Summit (NAIIS)
Outlines the National Adult and Influenza Immunization Summit’s (NAIIS) mission, opportunities for involvement, and resources aimed at healthcare professionals involved in adult and influenza immunization.
View ToolCampaign Planks
Provider & Staff Education
Clinical Support
IT / Documentation
Patient Education
