Research Posters

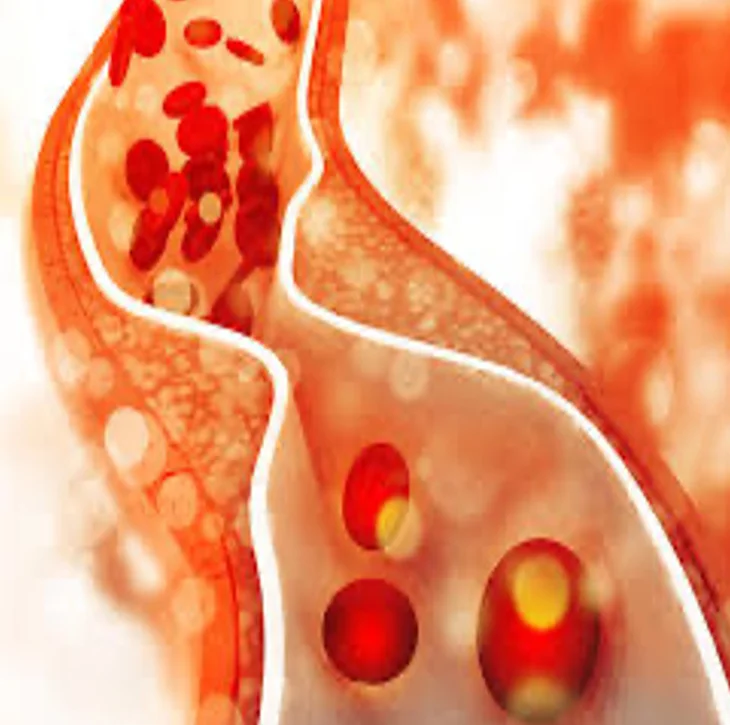
Lower Extremity Peripheral Artery Disease (PAD): Early Diagnosis and Treatment and Health Disparities
A deliberate, focused effort is necessary to close gaps and accompanying disparities in early evaluation, diagnosis, and treatment of people with lower-extremity peripheral artery disease (PAD). This poster describes approaches to improve care for this high-risk population.

Continuous Glucose Monitors: Implementation in Primary Care for Patients with Type 2 Diabetes
Use of continuous glucose monitors (CGMs) is increasing among patients with type 2 diabetes mellitus (T2DM). This poster examines effects of real-time CGM in real world settings on glycaemia in primary care patients with T2DM, particularly those not on intensive insulin therapy.

Implementation of "MIND at Home Program" in Primary Care for People Living with Dementia
As the U.S. population ages, the number of people living with dementia continues to grow. This poster presents results from an NIA pilot study for a home-based care coordination program integrated into primary care that addresses challenges of caring for this vulnerable population.
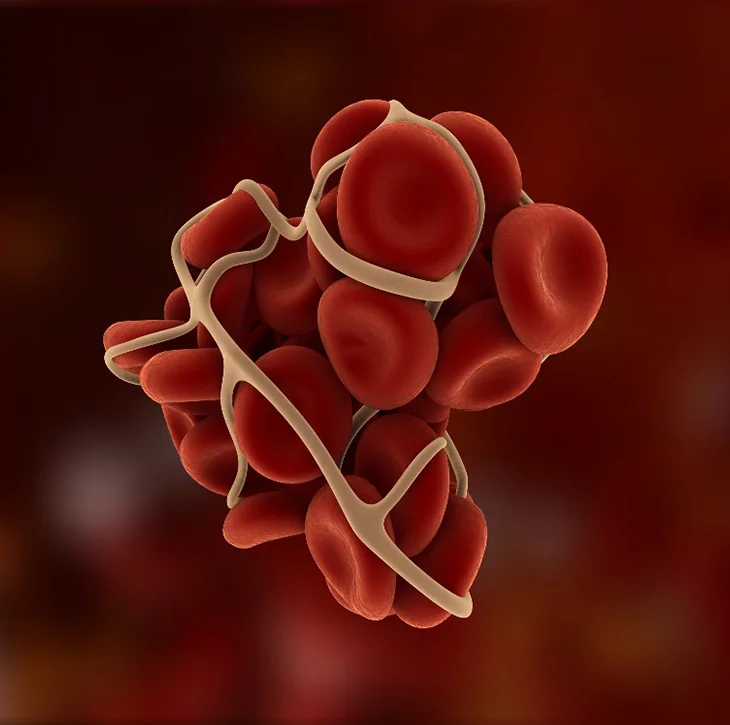
Case Study: Enhancing Care Transitions for Patients with Venous Thromboembolism (VTE)
Anticoagulants used to treat VTE are associated with bleeding and recurrent VTE events secondary to inadequate dosing or non-adherence to treatment plans. These medication outcomes are implicated as a major cause of VTE related hospital readmissions. This poster describes the focused interventions of North Mississippi Health System to improve care transitions for patients with VTE.

Management of Resistant Hypertension: Barriers to Blood Pressure Control
Patients with resistant hypertension, requiring four or more anti-hypertensive medications to achieve blood pressure (BP) control, are at risk of developing comorbid conditions. This poster describes the results of semi-structured interviews with providers who manage resistant hypertension and provides context on controlling BP in this challenging patient population.
Targeted Interventions and Improvement on Opioid-Related Quality Measures
To address the opioid crisis, in 2016, the Centers for Disease Control and Prevention (CDC) released opioid prescribing guidelines focusing on pain management, opioid prescribing, and/or medication treatment of opioid use disorder (MOUD). This poster showcases Henry Ford Health Systems application of the CDC guidelines and positive outcomes associated with these implementation strategies.